This weekend, the biggest unexpected incident in our little family happened.
Olivia, our oldest who is three, had been coughing at bedtime for a couple of days. Her allergist had suggested that she may have asthma a few weeks before, but we weren’t really sure what the symptoms looked liked in Olivia. We gave her medicine on Wednesday evening. Thursday, she progressively had a more difficult time breathing, requiring higher doses at lower intervals.
Finally, near 10 p.m. Thursday, she woke herself up coughing. We gave her the dose we had increased to and it didn’t work. Labored breathing, wheezing, coughing. We spoke to the on-call doctor at her pediatric allergist’s office. Time to move.
https://twitter.com/Kraft/status/307359586984292352
As a kid, I went to the ER a few times. In every case, we waited in the waiting room for sometime. I went to the military clinic, so there was not an urgent care option (at least back then), so the emergency room was the after-hour solution. It was always a wait. A long, long wait.
When you take a child into an ER complaining of difficulty breathing, let’s just say things are different:
Desk Person: “Hi, what can we do you for today?”
Me: “My daughter is having difficulty breathing. The on-call doc at her allergist told us to come to the ER.”
Triage Nurse (overhearing us, comes over from her station): “When did this begin? What medications has she been administered?”
Me: “This immediate set of issues began about 24 hours ago. She had been responding to albuterol via neb, but we’ve had to increase the dose to X and decrease the interval throughout the day to Y.”
Triage Nurse (listening to her chest): “She’s tight.” (To another person) “Take her back.”
Desk Person (handing me a pencil and a scrap of paper): “Her name and date of birth.”
And that was it. We were in a room.

Again, as a child in a military emergency room, I didn’t have a high set of expectations in terms of user experience for the ER. This experience has taught me that if you need to bring a child to the ER or hospital and there is a children’s hospital within a reasonable distance, go there. One of the pros of purchasing our house where we did is that you can see the children’s hospital from our upstairs landing.
As soon as they gave her a quick assessment and hooked her up to an oxygen monitor, her RN opened up a package of bubble solution and started playing with Olivia, blowing bubbles throughout the exam room. You could see the uncertainty in Olivia’s face wash away.
They began treating her and, while her oxygen levels were always okay, it took quite a bit to get her breathing under control. As we went longer into the night, the doctor prepared me that they would admit her if the next attempt didn’t get her back to where they wanted to see her.
Olivia did well, in the beginning, partly because I failed to bring any toys or books with us, so she got to play on “Daddy’s Exus” (known to us as a Nexus).
It was hard to see Olivia there. As her treatments in the ER had to intensify, so did the monitoring. With the levels of medication they were giving her, there was a concern about her heart rate increasing too much, so she was on an EKG and an automatically-monitored blood pressure unit. Her oxygen levels were still being monitored and something else that I can’t recall now.

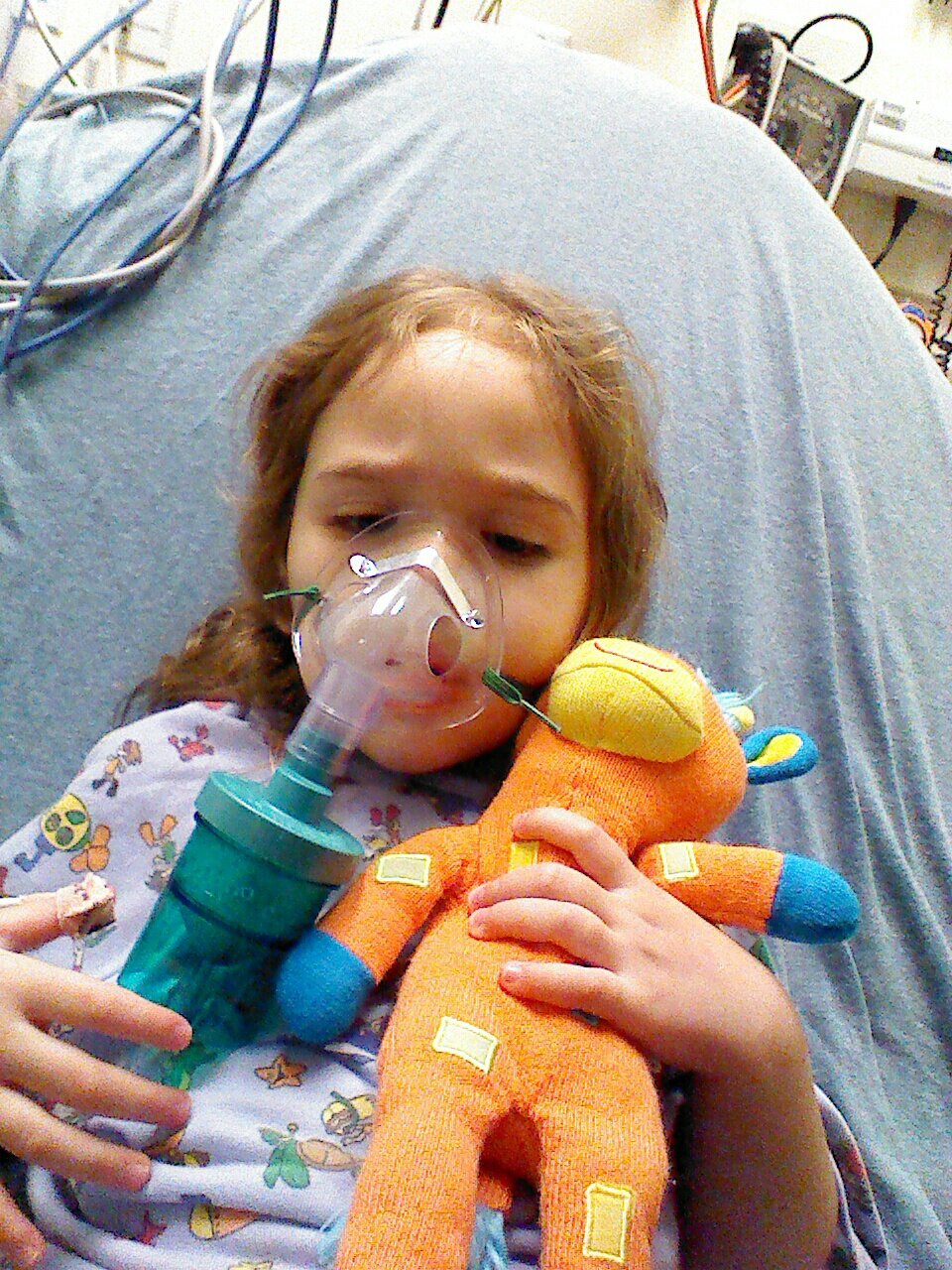
The hardest part, though, was when she finally fell asleep around 4:30 a.m. She was on her breathing mask, all of the various monitoring tools were wired to her. Granted, I’d been up since 6 a.m. the previous morning, trying to stay awake in her darken room. I was tasked with ensuring the mask stayed on her face if she moved. It was hard to be alone watching your child try to sleep like that.
Finally, around 6:30 a.m., the call was made to admit her. It took a few more hours to actually get her over to a room, but by the time they did, she was actually doing okay and didn’t require the constant mask or the monitoring.
https://twitter.com/Kraft/status/307469647245090816
The hospital experience, after that, was actually enjoyable. She was still in too bad of shape to go home, but she was past the worst of it. They let us explore the hospital and we found one of the playrooms open to patients and siblings.

The rest of the day progressed fine with slow, continual improvement. The call was made for one more night of observation since night time is the worst and she was showing displaying precursors to her last attack.
In the end, she improved and was released early afternoon on Saturday. In that time, I slept about six hours total, but she was happy, could breathe normally on a level of medication we could administer at home, and we were without the worry earlier in the week when this was an unknown, new thing for us.
https://twitter.com/Kraft/status/307938294312882176
Now, that Sunday night rolled around, I went back into a normal mode. Processed more e-mails that were skipped, checked out the project lists, todo lists, calendar and whatnot. Since I’m with the kiddos during the week, weekends are important times for my work schedule and this one was shot. I don’t care, though. Olivia is far, far, more important than anyone’s website or business, my own included.
The pro of being a freelancer in this situation is there was zero question on if I was taking the day off. The con, though, is next week won’t have any down time.
In the end, I can’t complain to have the work and and I can only celebrate having Olivia home.
Leave a Reply